
It is helpful to classify causes into vascular (non-thrombocytopenic) and thrombocytopenic disorders. Purpura is a sign rather than a diagnosis and a cause must be sought. Having inspected the skin and taken a history, it may be useful to return to a physical examination to reassess the purpuric rash and carry out a further systemic examination, looking for hepatomegaly/splenomegaly or neurological signs, for example. 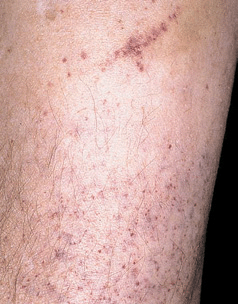 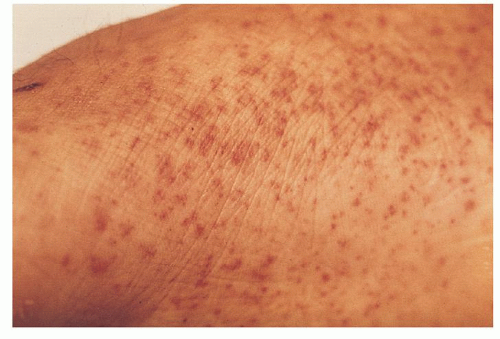
Other components of a routine history should be gone through (past medical history, medical and allergic history - including any over-the-counter drugs - and social history are all relevant). Recent travel history should be reviewed.Note whether general easy bruising has been noticed.That child may be moribund just 20 minutes later. If a child has developed a purpuric, possibly meningococcal, rash but does not seem unwell, do not be lured into a false sense of security. Establish whether the patient is otherwise well.Meningococcal septicaemia will be very recent in origin and changing almost visibly. Determine how long the rash has been present and whether it is changing noticeably.Leukaemia and myeloproliferative disorders can occur at any age. Senile purpura is confined to the elderly. Henoch-Schönlein purpura tends to occur in children. Tenderness may suggest an inflammatory process.Don't forget to ask/look for lesions in the mucous membranes.For example, localised lesions may be caused by trauma whereas purpura due to venous hypertension will be in the lower legs with a distribution as shown below. Note the nature of the lesions - size, confluence, associated blisters (and what these contain: exudate, blood, pus).In reality, the patient is likely to start the consultation by presenting with the purpuric rash and so inspection of the rash and noting such matters as the general condition of the patient will occur at the outset. It may seem unusual to place examination before history but there is some logic to this. The appearance of purpura is quite characteristic and it does not blanch on pressure. Nevertheless, clotting factor deficiency must be considered. As a general rule, purpura indicates a problem of the platelet system whilst a deficiency of clotting factors will cause haematomas or haemarthrosis as in haemophilia. Platelets help maintain the integrity of the capillary lining as well as being important in the clotting process. Purpura may occur with either normal platelet counts (non-thrombocytopenic purpuras) or decreased platelet counts (thrombocytopenic purpuras). Larger, deeper purpura are referred to as ecchymoses or bruising. When purpura spots are very small (<1 cm in diameter), they are called petechiae or petechial haemorrhages. Purpura is not a disease per se but is indicative of an underlying cause of bleeding. Purpura may also occur in the mucous membranes, especially of the mouth and in the internal organs. The term 'purpura' describes a purplish discolouration of the skin that is produced by small bleeding vessels near the surface.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
